For People Exploring Every Option Before Spine Surgery
Chronic Back Pain or
Sciatica?
You May NOT Need
Spine Surgery.
Before making a permanent decision about your spine, get a precise diagnosis and
find out whether minimally invasive, image-guided treatment is the right next step.
Most Major Insurance Plans Accepted
Same Week Appointments Often Available
Serving Lyndhurst, Paramus, Millburn, Edison, Flemington, Little Silver & Dover
Image-Guided
Precision
Same-Day
Procedures

Avoid Surgery
When Possible
We Accept
Most Major Insurance






Meet Dr. Timothy Calvert, MD
Board-Certified in Pain Management and Physical Medicine & Rehabilitation
Dr. Timothy Calvert is a board-certified interventional pain management physician and the Founder and CEO of the Institute of Orthopedics, Spine, & Sports (IOSS Medical). He holds dual board certification in Pain Medicine and Physical Medicine & Rehabilitation, and completed a fellowship in interventional pain management at Rutgers New Jersey Medical School — one of the leading accredited pain fellowship programs in the country.
Dr. Calvert's clinical philosophy is grounded in the belief that most patients with chronic spine pain deserve a thorough, evidence-based evaluation before surgery is considered. He combines advanced image-guided diagnostic techniques with a patient-centered approach — taking the time to review imaging, explain findings clearly, and map out a non-surgical treatment plan tailored to each individual's specific pain generator.
He is affiliated with Hudson Regional Hospital and Chilton Medical Center, and sees patients across seven IOSS Medical locations throughout New Jersey.
Credentials at a Glance:
Board-Certified, Pain Medicine — American Board of Physical Medicine and Rehabilitation
Board-Certified, Physical Medicine & Rehabilitation
Fellowship: Interventional Pain Management, Rutgers New Jersey Medical School
Residency: Physical Medicine & Rehabilitation, Temple University Hospital
Medical Degree: Drexel University College of Medicine
Before committing to spine surgery, patients deserve a comprehensive evaluation of all available options.


Appointments can be virtual or in person
How It Works

Step 1: Schedule Your
Evaluation
Book online or call
Same-week appointments often available
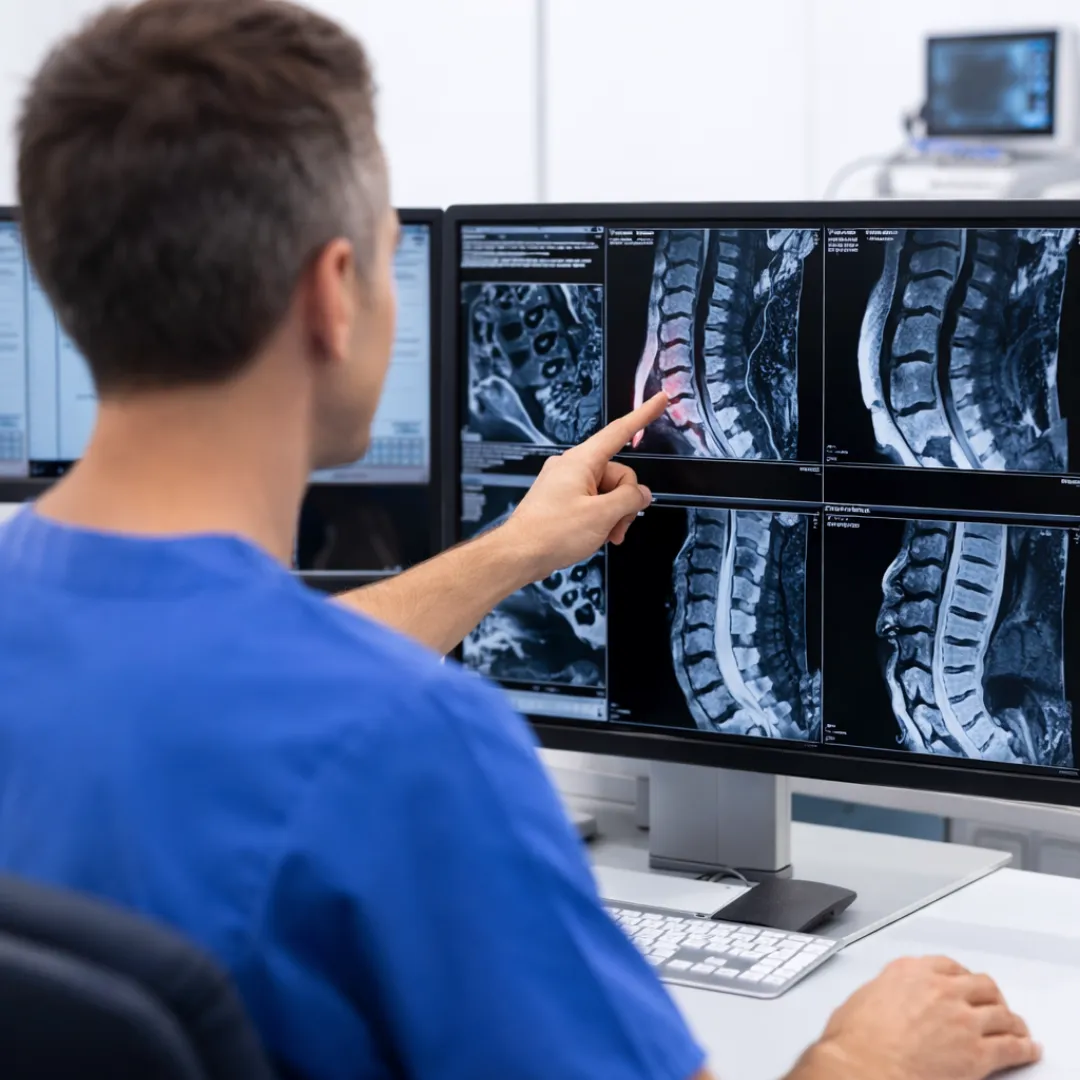
Step 2: Pinpoint the Pain Generator
MRI/imaging review + targeted exam
to identify what actually causing pain

Step 3: Treat Precisely
(If You're a Candidate)
Medial branch blocks, RFA, or epidural treatment based on your pain pattern
Appointments can be virtual or in person
Words from Our Clients
Real words from patients who saw incredible results with Dr. Calvert

Dr. Calvert and his team deliver exceptional care with personal attention every step of the way.
My daughter and I have been seeing Dr. Calvert for some time. I can not recommend his office enough. They are top notch! His staff, Mary and Paloma are both outstanding. Anytime I needed paperwork or a follow-up, they have both been on top of it and I can not thank them enough for that. Dr. Calvert has great bedside manner and doesn't treat you like a number as busy as he is. He spends the time with you and that means a lot. If I could give them ten stars, I would.
Mandy R.


Dr. Calvert and his team deliver exceptional care with personal attention every step of the way.
I can't say enough good things about Dr. Calvert. He is incredibly knowledgeable, patient, and thorough. He takes the time to listen to all concerns and explained everything in a way that was easy to understand. The staff is also friendly and efficient, making each visit a pleasant experience. I highly recommend Dr. Calvert to anyone looking for exceptional care!
Ella Berrian


Dr. Calvert listens, explains, and makes every visit feel comfortable and understood.

Dr. Calvert listens, explains, and makes every visit feel comfortable and understood.

Dr. Calvert is knowledgeable, thorough, and delivers real results that restore active lifestyles.
Highly recommend. I injured my knee during a half marathon a few years back and have had nagging pain ever since. It's something I had gotten used to, but it was keeping me from hiking and getting a good routine going at the gym. I had an amazing experience with Dr. Calvert. He is very knowledgable, thorough and provided a solid plan which has finally gotten me back to everything I want to do without pain!
Maya Patel


Dr. Calvert is knowledgeable, thorough, and delivers real results that restore active lifestyles.
Find Out if Dr. Tim Can Help You Virtually or in-person. No obligation, no card required
Do You Recognize These Symptoms?
You can’t stand or walk more than 15–20 minutes without needing to sit.
Your lower back feels stiff and “locked” in the morning.
Pain shoots down your leg when you cough, sneeze, or bend
Your MRI says “arthritis,” “disc bulge,” or “degenerative changes”
Physical therapy helped — but the pain always came back
You’ve been told surgery may be your only option
You're not imagining it.
And you're not out of options
Two Most Common Sources of
Chronic Spine Pain
Most chronic spine pain comes from either irritated facet joints or an inflamed spinal nerve.
Understanding the difference helps guide the right non-surgical treatment.
Facet Joint Arthritis
(“The Standing Pain”)
Deep ache across your lower back or belt line
Pain worse after standing 10–20 minutes
Sharp pinch when arching backward
Morning stiffness that improves slightly with movement
Relief when sitting or bending forward
Disc Herniation & Sciatica
(“The Leg Pain”)
Electric shock or burning down the leg
Numbness or tingling in the calf or foot
Pain worse when sitting
Can’t sleep comfortably
Sudden pain when coughing
Our Non-Surgical Spine Treatments
Minimally invasive procedures designed to diagnose and relieve the most common causes of chronic back and leg pain.
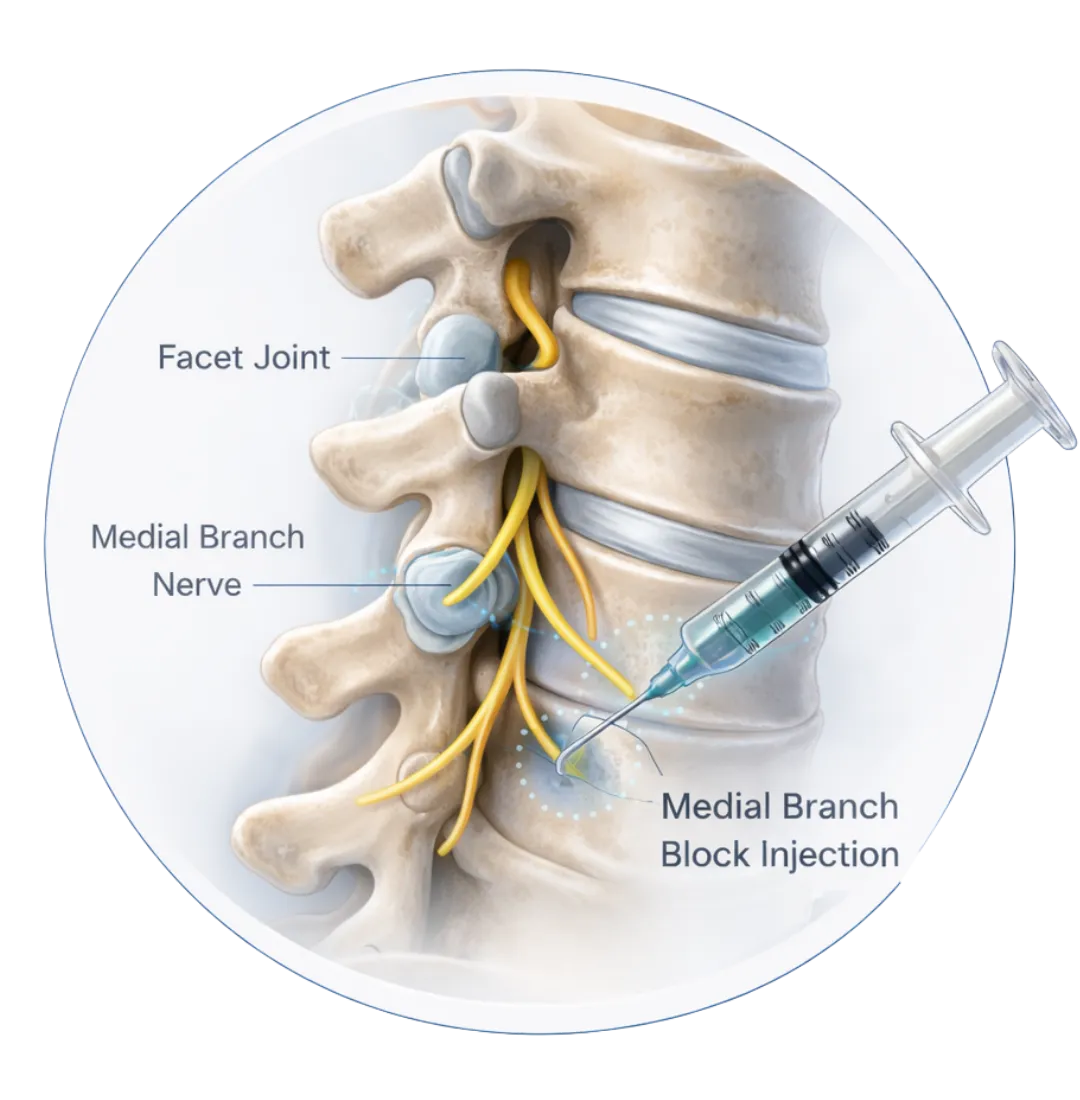
What Is a Medial Branch Block?
A medial branch block is a targeted diagnostic injection used to determine whether chronic back pain is coming from the facet joints of the spine. Under image guidance, a small amount of numbing medication is placed around the medial branch nerves, which carry pain signals from these joints.
If your pain significantly improves for several hours after the procedure, it confirms that the facet joints are the source. This allows us to move forward with a more definitive, longer-lasting treatment such as radiofrequency ablation — rather than guessing or rushing toward surgery.
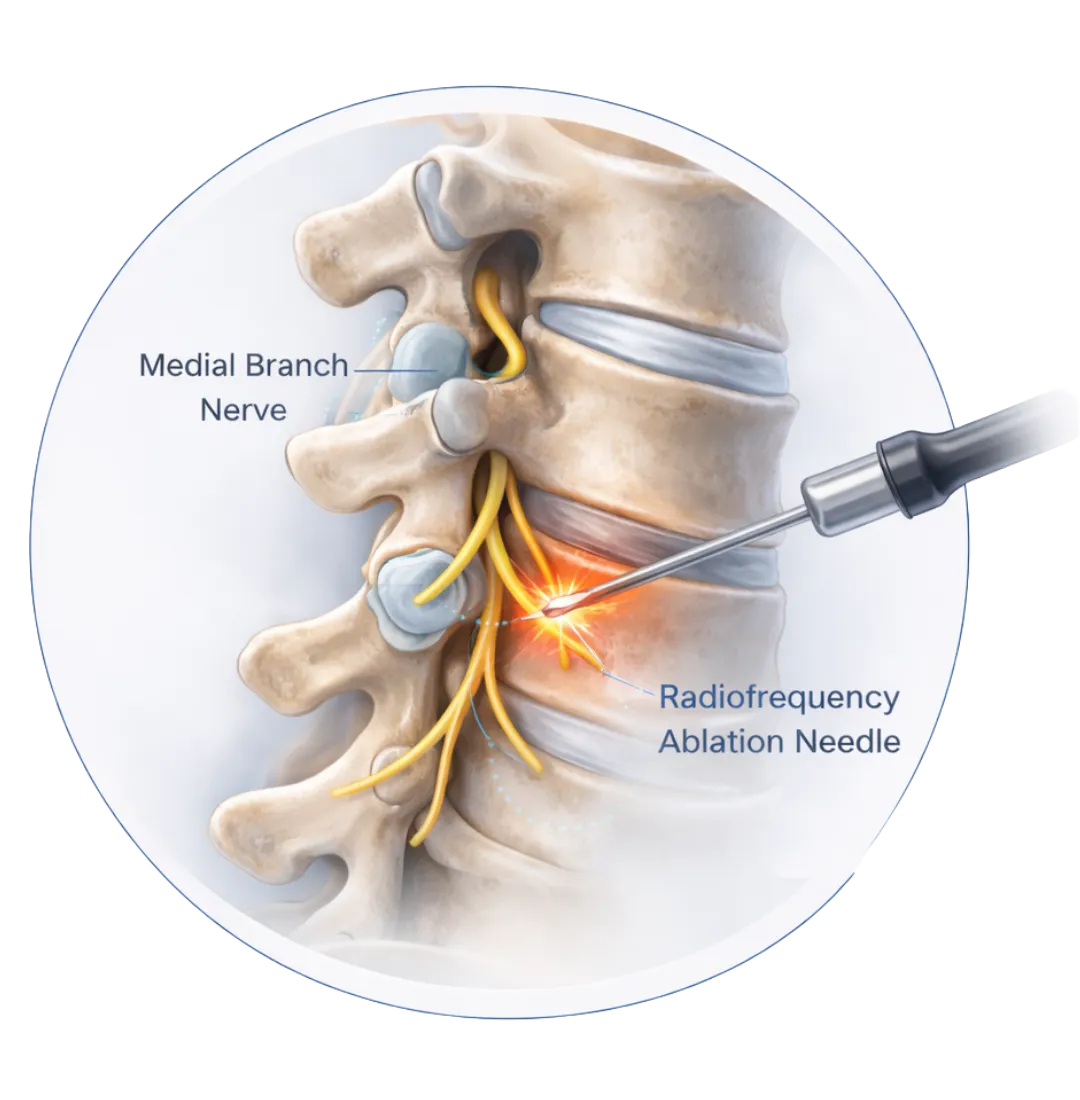
What Is Radiofrequency Ablation (RFA)?
Radiofrequency ablation is a minimally invasive outpatient procedure used to provide longer-lasting relief from facet joint pain. Using image guidance, a specialized needle delivers controlled heat to the medial branch nerves, temporarily disrupting the pain signals they transmit from the affected joints.
Because these nerves only carry pain signals — not strength or movement — the procedure does not weaken your spine. Relief often lasts 6 to 18 months or longer, depending on the individual. If pain returns as the nerves regenerate, the treatment can be safely repeated.
Radiofrequency ablation is typically recommended after a medial branch block has confirmed the source of pain, allowing us to treat the problem precisely and avoid unnecessary surgery.
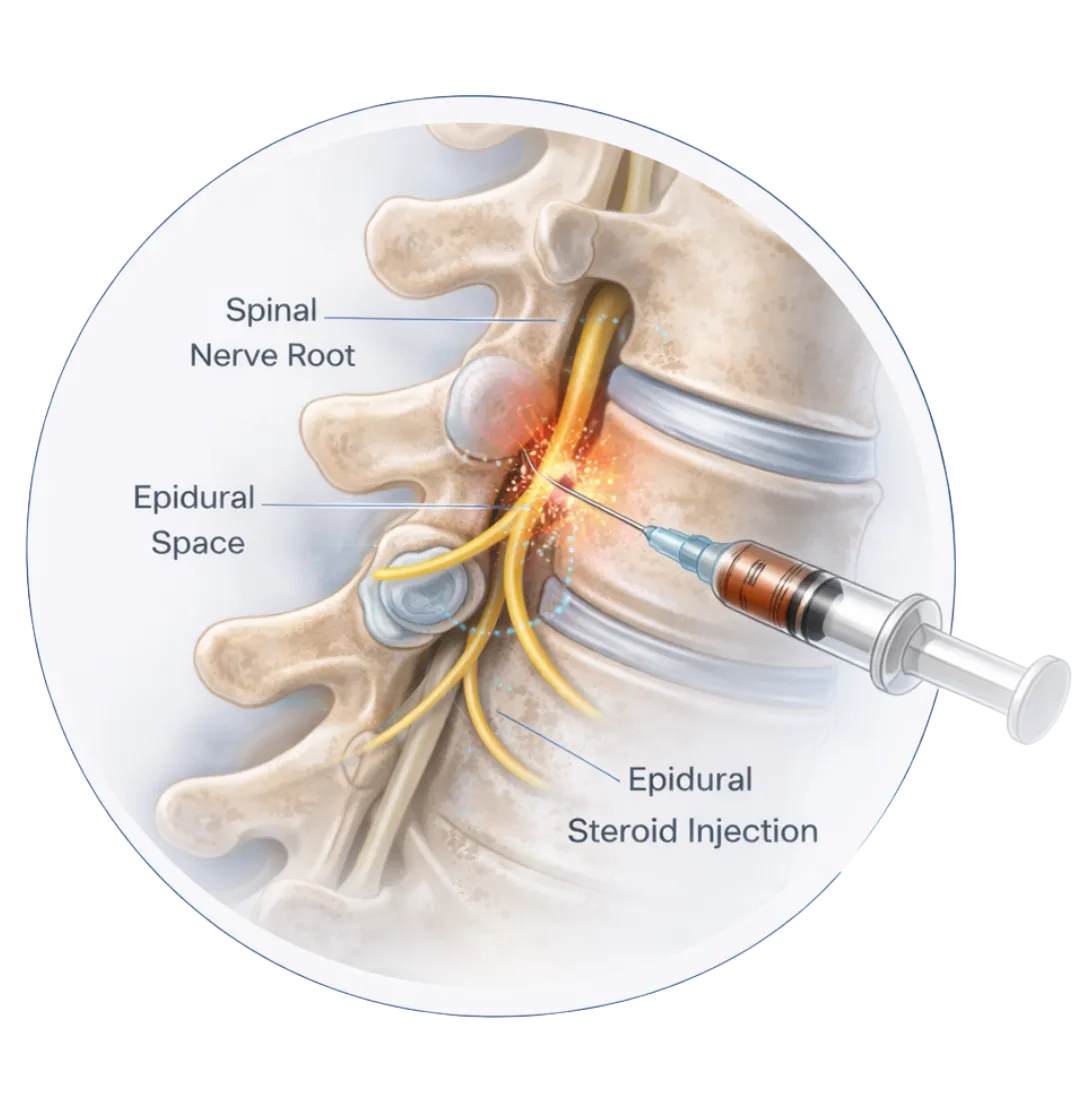
What Is an Epidural Steroid Injection?
An epidural steroid injection is a minimally invasive procedure designed to reduce inflammation around irritated spinal nerves. Using image guidance, anti-inflammatory medication is delivered into the epidural space surrounding the affected nerve root, targeting the source of radiating leg pain, numbness, or tingling.
When a disc bulge or herniation inflames a spinal nerve, the inflammation — not just the disc itself — often drives the pain. By calming that inflammatory response, epidural injections can significantly reduce symptoms, improve function, and in many cases help patients avoid or delay surgery.
Same-week appointments often available
Why Image-Guided Precision Matters
Content reviewed and accurate as of March 2026 by Dr. Timothy Calvert, MD.
When treating spinal nerves and facet joints, precision is everything — millimeters of needle placement can be the difference between effective treatment and missed target. Every procedure performed at IOSS Medical uses real-time fluoroscopic (X-ray) imaging to confirm exact needle position before any medication is delivered.
Without image guidance, injections rely on anatomical estimation and surface landmarks. Fluoroscopy allows Dr. Calvert to visualize the spine in real time, confirm needle depth and location, and treat the precise source of pain — improving both safety and outcomes. This is the standard of care recommended by the North American Spine Society (NASS) and the American Society of Interventional Pain Physicians (ASIPP).
Frequently Asked Questions
Q: Can I avoid spine surgery for chronic back pain?
Many patients with chronic back pain can avoid spine surgery, particularly when their pain is driven by nerve irritation, inflammation, or facet joint arthritis rather than structural instability. Minimally invasive, image-guided procedures such as medial branch blocks, radiofrequency ablation, and epidural steroid injections can provide significant and lasting relief for appropriate candidates. The key is accurate diagnosis — identifying the specific pain generator through a targeted evaluation and, when indicated, a diagnostic injection. Patients who want to exhaust all options before committing to surgery, those who have failed conservative treatment, or those who are not candidates for surgery due to health reasons are often excellent candidates for these non-surgical approaches.
Q: What is the difference between facet joint pain and sciatica?
Facet joint pain and sciatica are two distinct causes of spine-related pain that require different treatments. Facet joint pain originates from the small joints along the back of the spine that become arthritic or inflamed. It typically presents as a deep, aching pain across the lower back or beltline that worsens after standing 10–20 minutes, improves when sitting or bending forward, and is often accompanied by morning stiffness. Sciatica, by contrast, results from compression or inflammation of a spinal nerve root — usually from a disc herniation — and produces shooting, electric, or burning pain that radiates down the leg, often with numbness or tingling in the calf or foot. Sciatica typically worsens when sitting and can be triggered by coughing or sneezing. Because the treatments differ — RFA for facet pain, epidural injections for sciatica — accurate diagnosis before beginning any procedure is essential.
Q: Who is a good candidate for radiofrequency ablation (RFA)?
Good candidates for radiofrequency ablation are patients with chronic back or neck pain confirmed to originate from the facet joints — not from a disc herniation or structural instability. Candidacy is established through a prior diagnostic medial branch block: if pain decreases significantly for several hours after the block, the facet joints are confirmed as the source and RFA is appropriate. Ideal candidates have had pain for more than three months, have not found lasting relief from physical therapy or medications alone, and are not yet at the point where surgery is medically necessary. Patients with pacemakers, active infection, or bleeding disorders may not be suitable and should discuss their full medical history with Dr. Calvert during their evaluation.
Q: When is spine surgery actually necessary?
Spine surgery is typically necessary when a patient has a structural problem that cannot be addressed with injections or other non-surgical treatments, and when symptoms are severe enough to justify surgical risk. Clear surgical indications include progressive neurological deficits such as worsening weakness, loss of bladder or bowel control, cauda equina syndrome, spinal instability, or fracture. For most patients with chronic back pain, herniated discs, spinal stenosis, or sciatica, surgery is not the first or only option. Studies consistently show that a significant portion of patients told they need spine surgery achieve equivalent outcomes with appropriate non-surgical interventional care. A comprehensive evaluation — including imaging review and diagnostic injections — is the best way to determine whether surgery is truly necessary or whether a non-surgical path is appropriate.
Q: How long does radiofrequency ablation last?
Radiofrequency ablation typically provides pain relief lasting 6 to 18 months, and in some patients relief extends two years or longer. The duration varies based on anatomy, the specific nerves treated, and how quickly those nerves regenerate. Because RFA disrupts — rather than permanently destroys — the medial branch nerves, pain may gradually return as the nerves regrow. When this occurs, the procedure can generally be repeated safely with similar results. RFA is not a cure for the underlying arthritis or joint degeneration, but it is an effective and repeatable strategy for managing chronic facet joint pain without surgery.
Q: Are epidural steroid injections safe?
Epidural steroid injections are among the most widely performed interventional pain procedures in the United States and are generally considered safe when performed under image guidance by a trained specialist. Temporary side effects can include mild soreness at the injection site, brief flushing, or a short-term increase in pain before relief begins. Serious complications are rare. The use of real-time fluoroscopic (X-ray) guidance — used in every procedure at IOSS Medical — significantly improves accuracy and safety by confirming precise needle placement before medication is delivered. The risks and benefits are discussed in detail during your evaluation so you can make a fully informed decision.
Q: Does insurance cover medial branch blocks, RFA, and epidural injections?
Most major insurance plans — including UnitedHealthcare, Anthem, Blue Cross Blue Shield, and Aetna — cover medial branch blocks, radiofrequency ablation, and epidural steroid injections when medically necessary and properly documented. IOSS Medical accepts most major insurance plans and verifies your benefits before your appointment so there are no surprises. Call (908) 897-0655 or book online to begin the insurance verification process before your first visit.
Q: How quickly can I be seen by Dr. Calvert?
IOSS Medical prioritizes new spine evaluations and same-week appointments are often available across all New Jersey locations — including Lyndhurst, Paramus, Millburn, Edison, Flemington, Little Silver, and Dover. Appointments can be conducted in person at any location or virtually. Book online at youmaynotneedspinesurgery.com or call (908) 897-0655.
Appointments can be virtual or in person
Schedule Your Comprehensive Non-Surgical Spine Evaluation
In one visit, we review your imaging, identify the likely pain generator, and map your next best step — without rushing into surgery.
During your visit, we will:
Review your MRI or imaging
Perform a targeted physical exam
Identify the likely pain generator
Determine if you’re a candidate for diagnostic blocks, RFA, or epidural treatment
Clearly explain your options and expected timeline
Most major insurance accepted • Benefits verified before visit
• Same-week appointments often available
• Most major insurance accepted
• Benefits verified before visit
• Same-week appointments often available
Or Call (908) 897-0655
OFFICE LOCATIONS:
LYNDHURST:
1050 Wall Street West, #315,
Lyndhurst 07071
Phone: (908) 897-0655
PARAMUS:
275 Forest Ave #120,
Paramus, NJ 07652
Phone: (908) 897-0655
MILLBURN:
90 Millburn Ave #206,
Millburn, NJ 07041
Phone: (908) 897-0655
EDISON:
259 Talmadge Rd,
Edison, NJ 08817
Phone: (908) 897-0655
FLEMINGTON:
4 Walter E Foran Blvd #101,
Flemington, NJ 08822
Phone: (908) 897-0655
LITTLE SILVER:
200 White Road, #111,
Little Silver, NJ 07739
Phone: (908) 897-0655
DOVER:
57 Nelson Street,
Dover, NJ 07801
Phone: (908) 897-0655
The information on this page is for educational purposes only and does not constitute medical advice. Always consult a qualified physician before making decisions about your health or treatment. The procedures described on this page — medial branch blocks, radiofrequency ablation, and epidural steroid injections — are established, evidence-based interventional treatments endorsed by the North American Spine Society (NASS) and performed by board-certified specialists. This page is reviewed periodically for clinical accuracy. Last reviewed: March 2026.

